The normal cornea

- The air–tear interface is the most powerful refracting interface of the eye.
- The cornea is aspheric, with the central cornea steeper than the periphery.
- The refractive power of the optical zone (central 4 mm) is ≈43 D.
- The average adult transverse corneal diameter is 11–12 mm, and 9–11 mm vertically.
- Corneal clarity depends upon an ordered lamellar collagen structure and relative dehydration, requiring a minimum endothelial cell density of ≈1000 cells/mm2. The mean endothelial cell density falls by ≈0.6% per year.
- The central corneal thickness remains constant between the second and sixth decades but varies with the time of day (thickest in the morning) and race (Afro-Caribbeans and Chinese ≈530 μm, Caucasians ≈550 μm at 60 years).
- Normal corneal innervation is essential for the maintenance of an intact epithelial surface.
- The stem cells that generate the epithelium are located at the junction between the cornea and the sclera, probably in the palisades of Vogt.
- The normal cornea is avascular.
Dr. Khalid al Zubi lecture as power point presentations.
lecture video 1
conjunctiva lecture audio
History and Examination
History
- Ask about the presenting complaint, past ocular and medical history, medications, allergies, family, and social history. Document the presence or absence of the following key symptoms and determine their severity, nature, duration, and any relieving or exacerbating factors.
- Reduced vision.
- Abnormal sensation: direct stimulation of the corneal nerves usually gives rise to severe, sharp pain. Inflammation produces a dull, aching pain. Photophobia is a spasmodic pain on exposure to light caused by ciliary spasm. Irritation or grittiness is a symptom of epithelial disturbance. Itch usually indicates allergy. A diseased anaesthetic cornea may be asymptomatic.
- Tearing: multiple causes including corneal epithelial breakdown and stromal infl ammation.
- Red eye: ask if friends or family are affected, suggesting infection.
- Discharge: ask if this is purulent, mucoid, or ropey. Ask if friends or family are affected. Discharge is most often secondary to ocular surface infection or allergy.
- Contact lens: ask about contact lens wear including the type, cleaning routine, pattern of wear (i.e. daily or overnight), and duration of use
Examination
Corneal structure and function are dependent upon the lids, tears, conjunctiva, and sclera. Examine as follows, documenting relevant positive and negative findings.
General habitus, hands and face: for example, rheumatoid hand changes may help diagnose the cause of peripheral corneal thinning.
- Vision: record uncorrected, best-corrected, and pinhole VA. High-contrast Snellen VA may be maintained despite reduced contrast sensitivity from corneal opacity or
astigmatism. - Eyelids: note inflammation, abnormal contour, incomplete closure, misdirected lashes, and lid margin disease (blepharitis, meibomian gland plugging).
- Tears: note the quality (discharge, debris) and quantity (meniscus height). Measure tear break-up time (p. 158) if the tears appear abnormal, and tear volume with Shirmer I test.
- Bulbar conjunctiva: note scarring (location, extent) and subconjunctival haemorrhage. If inflamed, note depth (conjunctival, episcleral, scleral) and location (perilimbal, sectoral, diffuse, localized).
- Tarsal conjunctiva: evert the upper and lower lids to look for keratinization, scarring, foreign bodies (FBs), and the presence of membranes, papillae, and follicles.
- Corneal epithelium: note any defects (size, location, pattern, e.g. superficial punctate keratitis, dendritic, geographic), FBs, infiltrates (pattern, size, location, depth), oedema (extent and severity, e.g. bullae), deposits (location, pattern, material, e.g. iron, calcium, filaments).
- Corneal stroma: record the size, location, depth, and pattern of opacities. Infiltrates tend to have feathery margins. Scars have defined edges on retro illumination and often result in corneal thinning. Areas of oedema have soft, diffuse edges on retro illumination and increased corneal thickness. Note the depth, number of clock hours, and distance of corneal new vessels from the limbus. Ghost vessels carry no blood and appear grey. Inactive vessels may have blood flowing through them but appear to have sharp edges on retro illumination. Active vessels have a cuff of oedema producing a less-defined edge.
- Corneal endothelium and Descemet’s membrane: Note thickening, guttata, folds or breaks in Descemet’s membrane, and the extent and distribution of deposits (KPs, pigment, blood).
- Drawings: draw any corneal abnormities using a frontal and slit view. Baseline photographs may help quantify changes seen at subsequent examinations. Further clinical tests may be indicated based on the history and examination.
Investigations
Consider the following tests and investigations, as indicated by the history and examination.
- Corneal sensation: Corneal anaesthesia may be due to corneal disease or predispose to it. Warn the patient, and then lightly touch the peripheral cornea with a cotton-tipped bud. Compare sides.
- Vital dyes
- Fluorescein 2% Viewed with a cobalt blue light this fluorophore has multiple uses including:Tear film assessment Can be used to assess tear volume (meniscus height), quality (tear break-up time), and drainage (Jones tests and fluorescein disappearance test).
- Corneal disease Raised areas have a thinner layer of fluorescein over them and appear bluer. Thinned cornea with an intact epithelium ‘pools’ fluorescein, appearing green. Dead epithelial cells and exposed basement membrane stain green, e.g. corneal abrasion. Bowman’s layer stains slowly.
- Aqueous leakage (Seidel’s test) Fluorescein 2% is applied to areas of suspected leakage. The usually dark-orange 2% fluorescein is diluted by leaking aqueous, turning bright green under a blue light.
- Rose Bengal 1% should only be applied after topical anaesthetics. Warn patients that it may sting. Desiccated, devitalised conjunctival or corneal epithelial cells stain pink.
- Wash out afterwards with normal saline. Schirmer I test Bend a Schirmer strip at the preformed notch by 90° and place into the conjunctival sac at the junction of
the mid and temporal thirds of the lower lid, without using topical anaesthetic. Conduct the test in ambient lighting, with the patient blinking normally, eyes open and looking slightly up, and away from bright lights. Allow the paper to wet by capillary action.
Aqueous tear deficiency is diagnosed if the strip wets by ≤5 mm over 5 minutes. From 5 to 10 mm is borderline. The Schirmer II test uses topical anaesthetic before testing and has been used as a measure of ‘baseline’ tear production which is probably unphysiological, as all tear production is reflex.
Pachymetry Measuring the central corneal thickness (CCT) is useful for monitoring corneal grafts, prior to refractive surgery, and for normalizing IOP measurements. For normal values. There are several devices that measure CCT.
Bacterial Keratitis
Symptoms Unilateral red eye, discharge, tearing, and blurred vision. History Ask about onset, progression, treatment, level of discomfort, trauma, contact lens wear, and ocular or systemic disease.

Examination Examine adnexae, eyelids, conjunctiva, and cornea of both eyes for predisposing factors, e.g. dry eyes. Draw the size, location, depth, shape and colour of corneal infiltrate. Test corneal sensation. Perform Seidel’s test if perforation is suspected. Document anterior chamber cellular activity, including the size of any hypopyon. These are usually sterile unless Descemet’s membrane has been breached.
Differential diagnosis: Consider herpes simplex, acanthamoeba keratitis, or fungal keratitis, sterile peripheral infiltrates from contact lenses, and phlyctenular keratitis. Rarer causes of progressive infection include anaerobic bacteria (propionobacterium, capnocytophaga), Nocardia, mycobacterium (particularly post-LASIK), and microsporidia.
Management Perform a corneal scrape (bellow Box) to guide therapy, remove debris, and improve antibiotic penetration. Prescribe regular cycloplegia (e.g. G. homatropine 0.5% b.d.). If the cornea is thinned, apply a shield, without padding. Start empiric therapy with G. cefuroxime 5% and gentamicin 1% hourly, 30 mins apart, or alternatively G. ofloxacin 0.3% hourly in countries such as the UK, where quinolone resistance is rare.
Some streptococcal species are less sensitive to fluoroquinolones. Treat day and night for 2 days then day only. Admit if rapid onset, only eye, risk of perforation, or poor compliance. Otherwise, review with microbiology results in 2 days. If responding, continue treatment unaltered and review in a corneal clinic in 5 days. If improving at that visit, reduce antibiotics to q.d.s. and consider adding G. prednisolone 0.5% q.d.s. to reduce inflammation. Address any precipitating factors. If not responding, consider early
review, admission, re-scraping, and altering antibiotics based on sensitivities.
| Taking a corneal scrape 1. Liaise with microbiology staff. Request an urgent Gram stain. 2. Ask for chocolate agar, blood agar, Sabouraud agar 3. Instil G. proxymetacaine 0.5% then G. amethocaine 1%. 4. Explain the procedure. 5. At the slit lamp, use a Kimura spatula, No. 15 Bard Parker blade, or 20-gauge needle to remove superficial debris from the ulcer, and then scrape the edges and base. 6. Streak material onto two glass slides for Gram and Giemsa staining (or other preferred stain). Air dry and label with pencil. 7. Take additional scrapes, one for each culture medium. Streak material onto agar plates without breaking the surface. Flame the blade and cool for 20 seconds between scrapes, or select a fresh needle. 8. Plate onto blood agar, chocolate agar, and Sabouraud’s agar. 9. If acanthamoeba is suspected, streak onto the centre of a nonnutrient agar plate. 10. Tape covers onto the plates to prevent evaporation. 11. Inoculate brain–heart infusion and cooked meat broth by agitating the blade or needle in the media, (or by dropping a sterile cotton swab into the media). 12. Culture contact lenses, cases, and solutions. Document that the patient understands these will be destroyed in the process. 13. Label all material, and transport immediately to the laboratory. 14. Cultures may be positive in 24 hours, but can take up to 3 weeks for fungi, acanthamoeba, or anaerobes. |
Fungal Keratitis

History
Ask about ocular or systemic disease: candida keratitis is commonest in debilitated patients or those with preexisting corneal disease. Ocular trauma is associated with filamentous fungi, e.g. Aspergillus or Fusarium spp. Symptoms Unilateral red eye, tearing, and blurred vision. Pain and photophobia are initially mild, but become severe relative to the clinical signs.
Signs
The corneal surface typically appears grey with a dry rough texture. Filamentous fungi classically grow in a feathery branching pattern, but may be very rapidly progressive and indistinguishable from bacterial keratitis. Candida produces a small ulcer with expanding infiltrate in a collar-stud configuration, often superimposed on a debilitating corneal condition. There may be an endothelial plaque under the lesion
and satellite lesions at the edges. Suppurative keratitis, fibrinoid uveitis, hypopyon, and elevated IOP may occur.
Differential diagnosis Herpes simplex virus, acanthamoeba, and atypical bacterial keratitis, e.g. Nocardia, Mycobacterium, Propionibacterium.
Investigations
Take a corneal scrape for smear and culture. The diagnosis can often be made with the smear. Liaise with the microbiologist. If culture negative after 7 days and the patient is not responding, perform a partial-thickness corneal biopsy. This must be large (3 mm) and deep enough to include the affected areas. Send half to microbiology, half in formalin to histology. If available, in vivo confocal microscopy may be diagnostic.
Treatment
■ Discontinue any steroid treatment immediately.
■ Candida keratitis: G. amphotericin 0.15% (from i.v. preparation) hourly for 5 days then reducing to 4–6 times daily until the disease resolves. Use systemic treatment for peripheral or deep corneal ulceration (e.g. fluconazole 400 mg p.o. stat then 200 mg daily p.o. or i.v.). The frequency of topical therapy is as for candida keratitis above.
■ Filamentary fungal keratitis: G. amphotericin (as above) or G. econazole 1%, and itraconazole 100 mg b.d. for deep or peripheral lesions.
■ Shield without pad if the cornea is thinned.
■ Treat raised IOP.
■ Provide cycloplegia and analgesia as required.
Follow-up
Initially 1–2 times weekly until there are signs of improvement or deterioration halts. This may take days or weeks. A minimum of 12 weeks’ therapy is required for deep infection. Topical steroids are contraindicated in filamentary fungal infection as they promote fungal growth. Consider keratoplasty if the disease progresses after 2 weeks of optimal therapy; persisting with conservative treatment in this situation will lead to intraocular invasion (without perforation). A therapeutic penetrating keratoplasty is required in ≈25%, enucleation in 3%. Steroids should not be introduced after keratoplasty for 1–3 months because of the risk of recurrance in the host corneal ring.
Continue antifungals 4 times daily for several weeks after therapeutic keratoplasty.
Acanthamoeba Keratitis

Most (85%) cases occur in contact lens wearers. Protozoa may be isolated from contact lenses, water (fresh, salt, tap, swimming pools, hot tubs), dust, soil, or sewage.
History
Ask about contact lens cleaning regimen, swimming and showering in lenses, and the use of tapwater to clean lenses. Initially, pain and photophobia are mild; later they are often, but not always, severe relative to the clinical signs.
Examination
Signs are usually unilateral and highly variable. The cornea may show superfi cial punctate keratitis, reduced sensation, and dendritiform lesions. Perineural infi ltrates may be peripheral or central. Stromal infi ltrates are initially minimal, patchy, and widespread. Focal lesions are uncommon. Paracentral infiltrates may coalesce to form characteristic ring infiltrates. Other features include disciform oedema, scleritis, and mild uveitis. Hypopyon suggests bacterial superinfection.
Differential diagnosis Herpes simplex, fungal, or bacterial keratitis (e.g. Nocardia).
Investigations
A corneal scrape must be taken. Culture contact lenses, cases, and solutions. Explain that these will be destroyed in the process. A corneal trephine biopsy may be necessary in culture-negative cases that progress. Confocal microscopy, if available, can be diagnostic.
Treatment
Acanthamoeba cysts are highly resistant and in vitro susceptibility correlates poorly with in vivo activity.
■ First line: G. PHMB 0.02% or G. chlorhexidine 0.02% hourly, as signs of resolution appear reduce to q.d.s.
■ Second line: add G. propamidine 0.1%, G. hexamidine 0.1% or G. metronidazole 0.5% (from i.v. preparation) hourly.
■ First and second line drugs are often combined (G. PHMB 0.02% with G. hexamidine 0.1%).
Provide NSAID analgesia. Consider oral steroids and ciclosporin for painful scleritis resistant to treatment with NSAIDs.
Follow-up :
1–2 weekly until signs of resolution occur, then monthly as treatment is tapered off. Delay topical steroid use for at least 2 weeks as this may interfere with macrophages activity required to clear cysts. Do not use steroids if the inflammation is subsiding spontaneously.
Viral conjunctivitis:
Etiology: Conjunctivitis may accompany the common cold and other systemic viral infections (especially measles, but also chickenpox, rubella, and mumps). Localized viral conjunctivitis without systemic manifestations usually results from adenoviruses and sometimes enteroviruses or herpes simplex virus.
Epidemic keratoconjunctivitis usually results from adenovirus serotypes Ad 5, 8, 11, 13, 19, and 37 and tends to cause severe conjunctivitis. Pharyngoconjunctival fever usually results from serotypes Ad 3, 4, and 7. Outbreaks of acute hemorrhagic conjunctivitis, rare conjunctivitis associated with infection by enterovirus type 70, have occurred in Africa and Asia.
Symptoms and Sign: After an incubation period of about 5 to 12 days, conjunctival hyperemia, watery discharge, and ocular irritation usually begin in one eye and spread rapidly to the other. Follicles may be present on the palpebral conjunctiva. A preauricular lymph node is often enlarged and painful. Many patients have had contact with someone with conjunctivitis, a recent upper respiratory infection, or both.

Diagnosis
Diagnosis of conjunctivitis and differentiation between bacterial, viral, and noninfectious conjunctivitis (see Table: Differentiating Features in Acute Conjunctivitis) are usually clinical; special tissue cultures are necessary for growth of the virus but are rarely indicated. Nucleic acid amplification tests (NAAT) and other rapid, office-based immunodiagnostic tests, can be useful especially when the inflammation is severe and other diagnoses (eg, orbital cellulitis) must be ruled out. Features that may help differentiate between viral and bacterial conjunctivitis can include purulence of ocular discharge, presence of preauricular lymphadenopathy, and, in epidemic keratoconjunctivitis, chemosis. Patients with photophobia are stained with fluorescein and examined with a slit lamp. Epidemic keratoconjunctivitis may cause punctate corneal staining. Secondary bacterial infection of viral conjunctivitis is very rare. However, if any signs suggest bacterial conjunctivitis (eg, purulent discharge), cultures or other studies may be useful.
Treatment
Supportive measures
Viral conjunctivitis is highly contagious, and transmission precautions must be followed.
To avoid transmitting infection, physicians must
Use hand sanitizer or wash their hands properly (fully lather hands, scrub hands for at least 20 seconds, rinse well, and turn off the water using a paper towel)
Disinfect equipment after examining patients
Patients should do the following:
Use hand sanitizer and/or wash their hands thoroughly after touching their eyes or nasal secretions
Avoid touching the noninfected eye after touching the infected eye
Avoid sharing towels or pillows
Avoid swimming in pools
Eyes should be kept free of discharge and should not be patched. Small children with conjunctivitis should be kept home from school to avoid spreading the infection.
Viral conjunctivitis is self-limiting, lasting 1 week in mild cases to up to 3 weeks in severe cases. It requires only cool compresses for symptomatic relief. However, patients who have severe photophobia or whose vision is affected may benefit from topical corticosteroids (eg, 1% prednisolone acetate 4 times a day). Corticosteroids, if prescribed, are usually prescribed by an ophthalmologist. Herpes simplex keratitis must be ruled out first (by fluorescein staining and slit-lamp examination) because corticosteroids can exacerbate it.
Key Points
Most viral conjunctivitis is a highly contagious infection caused by adenoviruses or enteroviruses.
Features that may help differentiate between viral and bacterial conjunctivitis can include purulence of ocular discharge, presence of preauricular lymphadenopathy, and, in epidemic keratoconjunctivitis, chemosis.
Diagnosis is usually clinical.
Treatment is usually cool compresses and measures to prevent spread.
Herpes Simplex Keratitis:
Background Herpes simplex virus keratitis (HSVK) may occur as a primary infection in adults and children, but is more commonly due to reactivation of latent viral infection. Nonocular primary infection may be asymptomatic.
History:
Ask about potential triggers for recurrence such as UV light, trauma, cold, menstruation, psychological stress, systemic illness, and immunosuppression. Ask about previous labial, genital, or ocular HSV.
Examination
Test corneal sensation: hypoaesthesia occurs early. Examine the eye fully, as multiple sites may be involved.
■ Primary HSV : Common signs include eyelid rash (clear vesicles on erythematous eyelids and later crusting), conjunctival follicles (± pseudomembrane), punctate keratitis, subepithelial corneal infiltration or ulceration, dendritic ulcers, and disciform
lesions.
■ Recurrent HSV keratitis
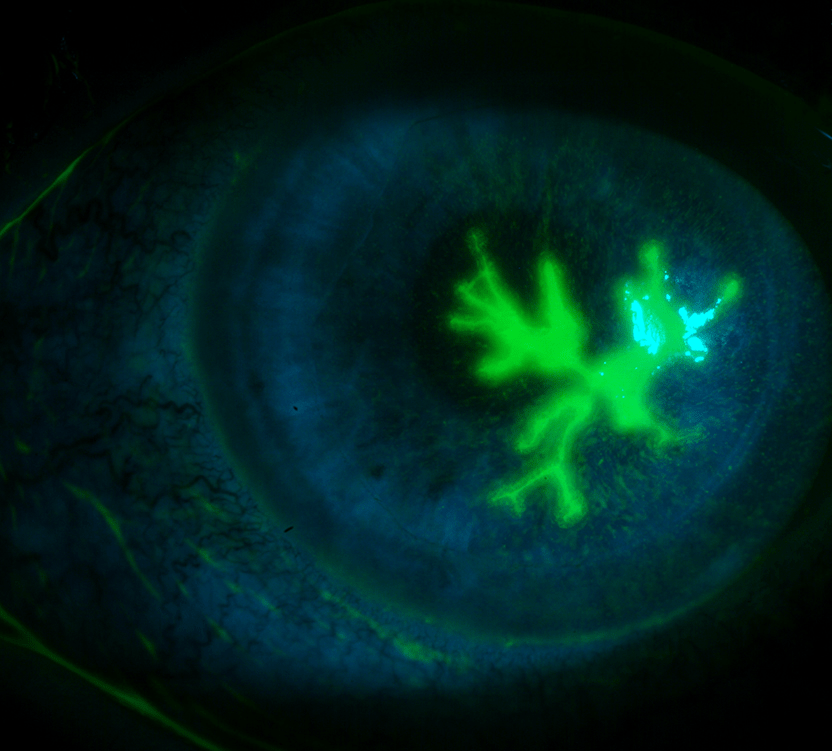
1. Epithelial HSV: Blotchy, stellate, or a filamentary keratitis usually progresses in 1–2 days to a classic dendritic pattern (branching lesions with feathery edges, and bulbs at the end). Fluorescein stains the ulcer and rose bengal stains the swollen epithelial cells at the ulcer’s edge. There may be underlying, slightly larger subepithelial ghost infiltrates. With prolonged infection or steroid use, a geographic or amoeboid ulcer may occur. There may be a mild anterior chamber cellular reaction.
2. Stromal HSV:
Three main patterns of disease exist:
a. Disciform ± endotheliitis: A circular area of oedema with minimal infiltrate or vascularization (except in recurrent disease). Fluorescein staining shows an intact epithelium, pushed forward by the underlying oedema. Oedema also produces folds in
Descemet’s membrane. Granulomatous KPs occur under the disciform or elsewhere. There may be anterior chamber cells and the IOP is often raised.
b. Necrotizing interstitial keratitis: typically shows intact epithelium, greyish-white stromal patches, corneal thinning, and neovascularization.
c. Necrotising interstitial keratitis with loss of the epithelium: beware rapid corneal melting. A hypopyon may occur with stromal necrosis or secondary to bacterial superinfection.
Differential diagnosis :
■ Epithelial disease: varicella-zoster keratitis, recurrent corneal erosion, healing abrasion, and contact lens pseudodendrite.
■ Stromal disease: other causes of interstitial keratitis, acanthamoeba, and bacterial keratitis.
Investigations Viral cultures have an approximate 70% recovery rate if taken within 2–3 days and prior to antiviral therapy (only 4% after treatment).
Treatment
■ Lid involvement
In the immunocompetent host, HSV is usually self-limiting. Lid lesions can be treated with warm compresses and Oc. aciclovir 3% t.d.s., or aciclovir 400 mg t.d.s. p.o.
■ Epithelial HSV
1. Debride loose epithelium using topical anaesthetic and a cotton wool swab. Instil G. homatropine 1%, Oc. chloramphenicol and pad overnight. Avoid if there is
stromal involvement.
2. Oc. aciclovir 3% five times daily for 14 days or for 7–10 days after healing. Treatment may initially aggravate subepithelial ghosting. This usually fades within a year and
does not require steroid therapy.
3. Treat mild uveitis with G. homatropine 1% b.d.
4. While ulceration persists use G. chloramphenicol q.d.s. as prophylaxis against bacterial superinfection.
5. Do not use topical steroids.
■ Stromal HSV
1. Steroids may be unnecessary for disciform HSVK as some episodes resolve spontaneously. Epithelial breakdown during steroid use can lead to rapidly progressive corneal thinning.
2. If steroids are necessary (e.g. failure of antiviral therapy, moderate to severe involvement, raised IOP) use G. prednisolone 1.0% q.d.s. or G. dexamethasone 0.1% q.d.s.
3. Prescribe Oc. aciclovir 5 times daily or aciclovir 400 mg t.d.s.p.o.
4. Prescribe G. chloramphenicol q.d.s. if there is an epithelial defect. Herpes simplex keratitis
5. Systemic steroids are not useful.
6. If epithelial healing has not occurred within 3 weeks, consider toxic or trophic epithelial defects. Change topical aciclovir to oral, and preserved topical steroids to
unpreserved.
7. Infection may be prolonged and damaging in immunocompromised patients.
8. Threatened or actual corneal perforation requires glue or tectonic keratoplasty. Penetrating keratoplasty has a high risk of HSV recurrence and rejection, so defer until the eye is uninflamed and steroid free. For recurrent corneal epithelial or stromal disease use aciclovir 400 mg b.d. p.o. for 1–2 years as prophylaxis. This reduces
recurrences by 50%.
Herpes Zoster Ophthalmicus (Ophthalmic Shingles)
Years to decades after primary varicella infection (chickenpox), latent virus in the trigeminal ganglion may reactivate. This produces eye disease and frontal/eyelid/nasal rash (ophthalmic division, V1).

Symptoms: Headache, fever, malaise, chills, and neuralgia. Ask about precipitating factors such as physical trauma, surgery, immunosuppression, and systemic illness.
Signs Multiple sites may be involved.
■ Skin/lids: crops of clear vesicles on inflamed hyperaesthetic skin with V1 distribution, typically occurring 2 days after neuralgia. Vesicular fluid becomes turbid and remains contagious until scabbed (Fig. 5.17). Occasionally dermatitis does not develop.
■ Conjunctiva: a follicular or papillary conjunctivitis is extremely common.
■ Episclera/sclera: focal inflammation.
■ Cornea: keratitis develops in ≈65% of patients, often with a marked decrease in corneal sensation and a varied appearance. Fine or coarse punctate epithelial keratitis occurs.
‘Dendrites’ differ from those of herpes simplex virus in that they are fine, greyish, nonulcerated. They stain poorly with fluorescein and lack terminal bulbs. Gentle debridement does not produce a fluorescein-staining ulcer, unlike HSV. Coarse, nummular, anterior stromal infiltrates may occur subsequent to epithelial disease. Neurotrophic keratitis occurs in ≈50%. Disciform, necrotic, interstitial or peripheral
ulcerative keratitis, or sclerokeratitis may occur.
■ Anterior chamber: 40% have cells and flare.
■ IOP: may be low, normal, or elevated. Marked elevation occurs in 10% (33% if keratouveitis).
■ Fundus: optic neuritis, central retinal vein occlusion, central retinal artery occlusion, necrotizing retinitis (acute retinal necrosis, ARN), thrombophlebitis, localized arteritis ±
exudates may occur.
■ Cranial nerves: palsies are not uncommon. Investigations HZO is a clinical diagnosis, but virus may be cultured from vesicles for 3–5 days. Take a careful history to exclude immunocompromise and investigate if suspected.
Acute treatment:
■ Aciclovir 800 mg 5 times daily p.o. for 7–10 days or famciclovir 500 mg t.d.s. p.o. for 7 days, ideally starting within 72 hours of onset.
■ Use skin toilet with or without topical disinfectants to prevent bacterial superinfection.
■ For epithelial defects prescribe Oc. chloramphenicol 1% q.d.s.
■ For iritis or moderate to severe disciform disease with intact epithelium use topical steroids commensurate with the severity.
■ If HSV is suspected, prescribe Oc. aciclovir 3% five times daily.
■ For unstable tear film or exposure keratitis add tear substitutes, e.g. unpreserved hypromellose 0.3% 2-hourly.
■ Offer appropriate analgesia and cylcoplegia as required.
■ For neurotrophic ulcers consider botulinum toxin protective ptosis or central tarsorrhaphy.
The use of systemic steroids, bandage contact lenses, tissue glue, tarsorrhaphy, and corneal grafts all require senior input, as do immunocompromised patients.
Treatment and follow-up of chronic disease
Corneal anaesthesia recovers fully in 60% in 2–3 months, but 25% develop permanent anaesthesia and neurotrophic keratitis. Disciform immune keratitis responds slowly and may require longterm, low-dose steroids to prevent recurrence. Skin lesions may
take weeks to heal, and leave scars.
Post-herpetic neuralgia (neuralgia lasting >6 months or >1 month after the skin heals) may be severe. Consider capsaicin cream 0.025% or 0.075% q.d.s. to affected skin. Burning sensation or erythema occurs in 30%. Capsaicin takes 2–3 weeks for onset of action. Taper frequency when pain relief begins at age <55 years with pain for < 3 months, stop 3–5 months after pain relief age >70 with pain >6 months, continue for 3 years. Restart if pain recurs on cessation. Amitriptyline may help (initially 25–50 mg p.o. once, increasing in 25 mg increments every 3–4 days until taking 75–100 mg). If the pain is uncontrolled with these treatments refer to a pain clinic.